Cardiac arrest occurs when the heart ceases to produce an effective pulse and circulate blood to the entire body. It may be caused by a cardiac electrical event such as ventricular fibrillation, progressive profound bradycardia, or when there is no longer a sustainable heart rhythm at all (systole).
Cardiac arrest may follow respiratory arrest; it may also occur when electrical activity is present but there is an ineffective cardiac contraction or circulating volume which is called pulseless electrical activity (PEA). Formerly called electrical-mechanical dissociation (EMD), PEA can be caused by any of the following disease process; hypovolemia (excessive bleeding), hypoxia, hypothermia, hyperkalemia, massive pulmonary embolism, myocardial infarction and medication overdose.
Clinical Manifestation
In cardiac arrest, consciousness, pulse and blood pressure are lost immediately. Ineffective respiratory gasping may occur, the pupils of the eyes begin dilating within 45 seconds. Seizures may or may not occur. The risk of irreversible brain damage and death increases with every minute from the time that circulation ceases. The interval varies with the age and underlying condition of the patient as well as the prompt emergency care provided by emergency responders in resuscitating the patient. During this period, the diagnosis of cardiac arrest must be made and measures must be instituted immediately to restore cardiac function and circulation.
Emergency management of cardiac arrest
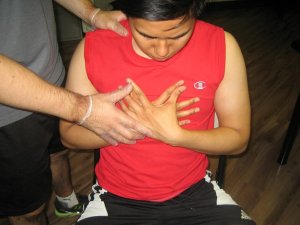
The most basic and possibly the most effective emergency management for cardiac arrest is prompt and proper initiation of cardiopulmonary resuscitation (CPR). CPR provides blood flow to vital organs until effective circulation can be re-established (usually upon arrival of emergency medical services with advance life support equipment). The ABCDs of basic CPR must be observed; airway, breathing, circulation and defibrillation in order for the individual to have a fighting chance for survival.
If the patient is already resuscitated, he/she must be constantly under strict monitoring with multifunction pads which are usually integrated in most defibrillators to monitor for electrical conductivity of the heart. Initially, when emergency respondents have arrived at the scene and no prior CPR has been initiated, CPR is only performed initially only if the defibrillation is not possible. The survival rate decreases significantly for every minute that defibrillation is delayed. If the patient has not been defibrillated within 10 minutes, the chances of survival are close to zero. The decision to terminate resuscitation is based on the medical considerations and takes into account the underlying circumstances as well as the chances of survival of the individual.
Follow-up monitoring and care of cardiac arrest
Once resuscitation was successful (emergency medical services were
able to revive the patient or the patient was brought to a medical facility on earliest possible time), the patient must be transferred to the intensive care unit for close observation and monitoring. Continuous ECG monitoring and frequent blood pressure assessments are essential until hemodynamic stability is re-established. Etiologic factors that may either limit or even aggravate the arrest, such as metabolic or rhythm abnormalities, must be identified and treated. Possible contributing factors such as acid-base imbalances need to be identified and corrected as early as possible in order to prevent additional medical problems from precipitating the already critical episode of cardiac arrest.
